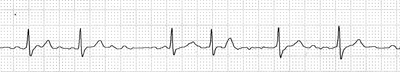
Atrial Fibrillation
Atrial fibrillation (AF) is a disorder that results in multiple wavefronts of reentry simultaneously circulating around the atria, giving the appearance of disorganized electrical activity of the atria. AF can be recognized on the ECG by an irregularly irregular ventricular rhythm with disorganized fibrillatory activity in the baseline. The incidence of atrial fibrillation increases dramatically with age, affecting 2-3% of patients in their seventies and 10-12% of patients over the age of eighty. It is also commonly seen in patients with valvular heart disease, ischemic heart disease, cardiomyopathy, and hypertension. Occasionally, atrial fibrillation occurs in the absence of underlying heart disease, and in those cases it is known as “lone” atrial fibrillation.
Atrial fibrillation results in a number of physiologic disturbances. First, the heart rhythm is often rapid and irregular, which can cause patients to experience palpitations. Also, the heart rate may increase dramatically with only mild physical activity, resulting in exertional shortness of breath and exercise intolerance. Shortening of left ventricular filling time caused by the rapid rate combined with the loss of the atrial “kick” results in a decrease in the cardiac output, which may also cause shortness of breath and exercise intolerance, as well as lightheadedness, low blood pressure, and fatigue. Patients with diastolic dysfunction (non-compliant or “stiff” ventricles) are particularly affected by the compromised LV filling and loss of atrial contribution to ventricular filling. Finally, the loss of an organized atrial contraction results in stasis of the blood in the atria, particularly in the left atrial appendage. This can result in the formation of a blood clot (thrombosis) that can break off and travel within the circulatory system (embolization). This can lead to a stroke, which is the major source of morbidity and mortality from atrial fibrillation. It is believed that 15% of all strokes occur as a result of atrial fibrillation. The risk factors for stroke in AF include age over 65 (especially over 75), hypertension, diabetes, vascular disease, history of heart failure, or a history of a prior stroke.
In the past, patients with AF were given warfarin to thin the blood, to inhibit blood clot formation and reduce the risk of stroke. Nowadays, warfarin is only required in patients with a mechanical heart valve replacement or with mitral stenosis. Most patients requiring anticoagulant medications to reduce the risk of stroke now receive one of the "newer" agents, which include apixaban, rivaroxaban, and dabigatran. These have been shown to be more effective and safer than warfarin in patients with "non-valvular" atrial fibrillation. These medications do not require frequent blood tests like patients on warfarin do. Patients with atrial fibrillation and increased risk of stroke should be anticoagulated indefinitely, as many large studies have demonstrated that this can reduce the risk of stroke by nearly 80%. The only patients who do not require anticoagulation are those with “lone” atrial fibrillation under the age of sixty-five. These patients appear to have a very low risk of stroke and can be managed with aspirin alone.
Patients presenting to the emergency room with new onset atrial fibrillation (less than 24 hours) with a rapid ventricular response should be treated initially with intravenous AV nodal blocking agents such as beta-blockers, verapamil, or diltiazem. Spontaneous conversion to sinus rhythm occurs in the majority of patients within 24 hours with just rate control. Digoxin is not effective under these circumstances. Once the ventricular rate has been controlled and the patient's symptoms have been relieved, electrical cardioversion or initiation of antiarrhythmic drugs for “chemical” cardioversion may be considered in patients who do not convert spontaneously, as long as the AF has been present for less than 24-48 hours. If the duration of AF exceeds 24-48 hours (or if the duration is unknown), the risk of embolic complications of cardioversion increases significantly. These patients should be anticoagulated for a minimum of three weeks before cardioversion can be performed safely. Patients needing more urgent cardioversion should have trans-esophageal echocardiography to rule out a left atrial thrombus. Once a clot has been ruled out, cardioversion can be performed while the patient is still sedated. Cardioversion, if done correctly, has a 98% success rate and a 0.5% risk of stroke regardless of whether a TEE is performed.
The use of antiarrhythmic drugs to maintain normal sinus rhythm after cardioversion is necessary in most patients, as atrial fibrillation is very likely to recur. However, the risk of side effects from these drugs is significant. Better long-term results seem to be achievable with catheter ablation for atrial fibrillation, especially with the recent development of "Pulsed Field Ablation" (PFA), which has now become the most commonly used ablation technique. PFA is about 80% effective for long-term suppression of AF. This procedure is shorter (only 1-2 hours) and safer than prior ablation techniques using radiofrequency (RF) electrical energy. Most of the time AF arises from the pulmonary veins on the back wall of the left atrium. Thus, the most common target for ablation are those veins. "Pulmonary vein isolation" is the goal in all AF ablation procedures, which means that the veins are electrically disconnected from the rest of the atria. This prevents any abnormal electrical activity in the vein from affecting the patient's rhythm. There remains a 1-2% risk of serious complications of AF ablation, including cardiac puncture, tamponade, phrenic nerve injury, systemic embolization, or even death. However, the PFA technique has essentially eliminated many other complications related to RF ablation, including pulmonary vein stenosis and atrio-esophageal fistula. Some patients still have to have a repeat procedure because of recurrent atrial fibrillation or flutter. Nevertheless, AF ablation continues to be an exciting and promising treatment for this otherwise frustrating condition.
